
Although the TIMI score was originally developed as a tool for patients with confirmed ACS ( 10), a low score has also been shown to identify ED chest patients with a low pre-test probability of ACS ( 2).Ĭarlton et al. The 2016 update of the National Institute for Health and Care Excellence (NICE) Chest Pain of Recent Onset guidelines however state that this approach should only be used in patients identified as low risk by a validated tool, such as the TIMI score ( 9). This approach is therefore recommended (class 1) by the European Society of Cardiology guidelines ( 8). The use of a presentation hs-cTn below the limit of detection (LoD) of the assay in patients without signs of acute ischemia on their ECG has a very high negative predictive value (NPV) for AMI ( 6, 7). The now commonly used high-sensitivity cardiac troponins (hs-cTn), have an improved analytical and diagnostic sensitivity compared to previous generations of cTn, and enable faster rule-out of AMI ( 5). There is thereby room for significant improvement in our assessment of chest pain patients. In the end however, less than 25% of all admitted chest pain patients prove to have ACS ( 2, 4). The fear of missing cases of ACS leads to lengthy ED assessments and high admission rates for serial troponin samples and non-invasive testing or coronary angiography ( 2, 3). The list of differential diagnoses is long, but it is normally the perceived likelihood of acute coronary syndrome (ACS), i.e., acute myocardial infarction (AMI) or unstable angina (UA) that drives management. Received: 10 January 2018 Accepted: 20 January 2018 Published: 21 January 2018.Ĭhest pain is a common complaint among patients at the emergency department (ED) and accounts for about 5–10% of all ED visits ( 1). Assessment of the 2016 National Institute for Health and Care Excellence highsensitivity troponin rule-out strategy. Email: on: Carlton EW, Pickering JW, Greenslade J, et al. 
Department of Internal and Emergency Medicine, Department of Cardiology, Skåne University Hospital, Klinikgatan 15, 221 85 Lund, Sweden. Policy of Dealing with Allegations of Research MisconductĬorrespondence to: Arash Mokhtari.Policy of Screening for Plagiarism Process.The TIMI risk score may be a useful tool for risk stratification of ED patients with chest pain syndrome. Overall, the score had similar performance characteristics to that seen when applied to other databases of patients enrolled in clinical trials and registries using a 14-day end point. The highest correlation of an individual TIMI risk indicator to adverse outcome was for elevated cardiac biomarker at admission. The TIMI risk score at ED presentation successfully risk-stratified this unselected cohort of chest pain patients with respect to 30-day adverse outcome, with a range from 2.1%, with a score of 0, to 100%, with a score of 7. 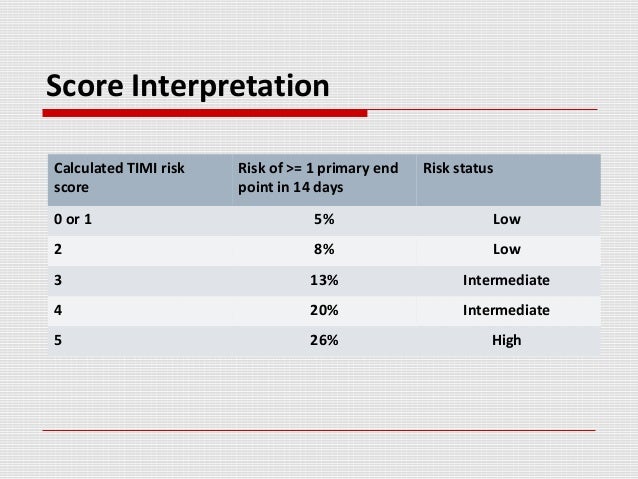
The main outcome was the composite of death, acute myocardial infarction (MI), and revascularization within 30 days. These patients had TIMI risk scores determined at ED presentation. Although validated and used frequently in patients already enrolled in acute coronary syndrome trials, the Thrombolysis in Myocardial Infarction (TIMI) risk score never has been examined for its value in risk stratification in an all-comers, non-trial-based ED chest pain population.Īn analysis of an ED-based prospective observational cohort study was conducted in 3,929 adult patients presenting with chest pain syndrome and warranting evaluation with an electrocardiogram. 
Prompt and accurate risk stratification to identify those patients with NSTE chest pain who are at highest risk for adverse events is essential, however, to optimal management. Patients presenting with chest pain or related symptoms suggestive of myocardial ischemia, without ST-segment elevation (NSTE) on their presenting electrocardiograms, often present a diagnostic challenge in the emergency department (ED).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
